By Margaret Songy, Pharmacy Resident, Baptist Health-North Little Rock
What is defined as a fever?
A fever is when the body temperature is higher than the normal core temperature of 100 degrees Fahrenheit (37.8 degrees Celsius). Normal body temperature can fluctuate, ranging from 97.5 degrees F (36.4 degrees C) to 98.9 degrees F (37.2 degrees C).
The presence of fever is often a cause for concern among patients and caregivers, and pharmacists can be an excellent resource for those seeking guidance regarding the use of nonprescription antipyretics.
Below is a chart for reference comparing the differences in body temperature when measured at different sites.
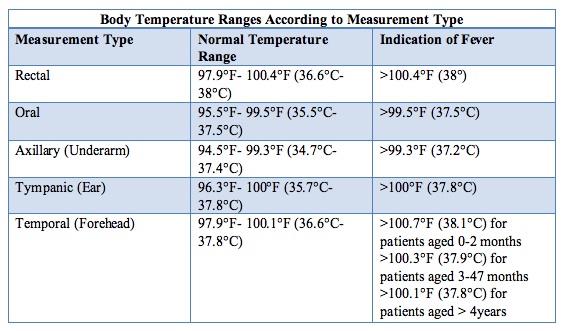
Causes & symptoms
Fever can result from factors such as an infectious process, a response to the use of certain medications (also known as a drug fever), or it can be unknown in origin. Fever can also occur after the administration of common childhood immunizations. However, most fevers are caused by microbial infections such as bacterial, viral, fungal, and yeast infections.
Patients with fever may experience signs and symptoms that can cause discomfort including headaches, facial flushing, chills, sweating, and joint or muscle pain.
Treatment options
The primary goal in the treatment of fever is to relieve discomfort by returning body temperature to normal. It is also important to identify and treat the underlying cause of fever.
Most fevers can be managed easily with proper treatment, but sometimes fever may indicate a serious underlying illness such as an acute infection that requires immediate evaluation and treatment.
Nonprescription fever-reducing and non-pharmacologic measures are often used in the treatment and management of fever. Available nonprescription medications that help to reduce fever include acetaminophen (Tylenol) and non-steroidal anti-inflammatory medications, including aspirin, ibuprofen (Advil), and naproxen (Aleve).
Acetaminophen and ibuprofen are the two most extensively used fever-reducing medications. However, ibuprofen is only approved for fever reduction in patients older than 6 months. Fever-reducing medications are available in a variety of formulations for the adult and pediatric patient population making administration easier.
Typically, temperature decrease and alleviation of discomfort occur about 30 to 60 minutes after administration of medication. Non-pharmacologic measures such as adequate fluid intake to prevent dehydration, wearing lightweight clothing, and maintaining a comfortable room temperature should also be incorporated in treatment.
Ways to check your temperature
It is best to avoid feeling the forehead to check for fever. Instead, use a reliable thermometer and follow the manufacturer’s recommended procedures to obtain an accurate reading.
- Digital thermometers are the most widely used measuring devices, and are available with a variety of features enabling temperature measurement via the mouth, ear, under-arm region, rectum, or forehead. During the course of an illness, temperature should be measured with the same thermometer at the same site in order to obtain consistent measurements.
- Use of a rectal thermometer is the preferred method for temperature measurement in patients 6 months and younger. Tympanic (ear) thermometers are not recommended for this age group because of the shape and size of an infant’s ear.
- While measuring temperature rectally is preferred for patients aged 6 months to 5 years, oral, tympanic, or temporal temperature measurement may be used in this patient age group if proper technique is used.
- In patients older than 5 years, oral, tympanic, or temporal temperature measurement is adequate.
If symptoms continue and you need help from a medical professional, you can request an appointment with a Baptist Health provider.

